Dec 2004
Gastroesophageal Reflux
and Down Syndrome
by Len Leshin, MD, FAAP

Copyright 1997, 2004 All rights reserved

Gastroesophageal Reflux (GER) is probably the most common gastrointestinal problem in childhood. GER is defined as the movement of contents of the stomach (solids or liquids) into the esophagus. Commonly, this results in children "spitting up" or even forcefully vomiting. While some spitting up in infants is common and may even be called normal, it becomes abnormal when it causes either distress in the child or complications to the child's health such as pneumonia, esophagitis or slow growth.
|
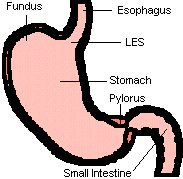
The cause of GER is most often a decrease in function of the lower esophageal sphincter (LES), a muscle that lies at the junction of the esophagus and stomach. This muscle is supposed to keep stomach contents in the stomach, but in GER, normal contracting of the stomach during digestion propels some stomach contents back up the esophagus. Mostly this is a problem with the tone of the LES. However, posture of the infant can also affect the LES, as being "slumped over" in an infant seat or lying down on the back can increase the reflux.
Another contributing factor to GER is how much the stomach holds and how fast it empties out into the small intestine, as infants with smaller stomachs and slower emptying times tend to reflux more than any other age group. |
Signs and Symptoms
The most obvious signs of reflux are frequent spitting up and/or vomiting. While normal infants may spit up occasionally, the infant with reflux will spit up or vomit after almost every feeding. The difference between spitting up and vomiting is one of force: vomiting is more forceful, usually due to spasms of the pylorus muscle. 85% of all infants with GER will show signs by 7 days of age, with another 10% showing signs by the 6th week of life.
Some infants and children will have GER but the stomach contents won't come up all the way to the mouth. Others will have just enough contents come up that they will have to swallow again, but not spit up or vomit. One condition called Sandifer syndrome presents with swallowing actions and an unusual head tilt, and reflux that may or may not be obvious. Any infant that seems to be continuously choking, gagging or making swallowing noises should be evaluated for GER.
For reasons that aren't entirely clear, GER can produce apnea in infants. Apnea is the temporary absence of breathing, usually lasting 10 to 20 seconds, and sometimes accompanied by a bluish color of the face.
GER can also cause respiratory symptoms when stomach contents coming back up the esophagus trickle over into the airway. This can cause a chronic cough, a hoarse noise during breathing ("stridor"), wheezing, and repeated cases of pneumonia.
GER also can cause chest pain, often referred to as indigestion or heartburn. This is because the stomach contents become acidic after exposure to the gastric acid, and the lining of the esophagus isn't meant to be exposed to stomach acid. In some infants this discomfort is registered as prolonged fussiness or crying, and may be one cause of infant colic. If untreated, the GER can eventually cause esophagitis, which is an irritation of the walls of the esophagus. Severe esophagitis may lead to bleeding and scarring of the esophageal lining.
Diagnosis
In most cases, the diagnosis of GER is fairly obvious. For less obvious cases, the usual means of diagnosis is through radiological tests. One test, the Upper GI, involves the infant or child swallowing barium, a radio-opaque liquid. ("Radio-opaque" means that the liquid shows up as white on Xrays, not that the substance is radioactive.) Several Xrays are taken as the infant swallows to see if any liquid comes back up, and how far up it comes in the esophagus. However, because GER is an episodic event, the Upper GI test may not always catch the reflux; so a negative test does not prove the child doesn't have GER. (Note that an Upper GI is not the same as a "Barium Swallow" test. The Barium Swallow only looks at esophageal function and may not catch episodes of reflux that an Upper GI test will.)
Another Xray test is Scintigraphy, also called a "gastric-emptying test" or a "milk scan." In this test, the infant or child is fed a liquid that has a very small amount of technetium, a compound that can be seen by special equipment. While this test takes longer to do than an Upper GI, it involves a smaller amount of radiation exposure to the infant. This test has the advantage of observing the child over a longer period of time and may pick up cases of GER that the Upper GI might miss.
In more difficult cases, the esophagus may need to be looked at directly for signs of irritation to the lining. This is done by endoscopy, in which the doctor puts a fiber-optic tube down the sedated child's throat to examine the esophagus. If necessary, biopsies can be done at this time, which is the removal of a small piece of esophageal lining to be looked at under a microscope later.
Finally, in cases where a definitive diagnosis is elusive or when surgery is being planned. an esophageal pH probe may be done. In this situation, the child is observed in the hospital overnight with a probe placed in the child's esophagus. This probe will measure the pH of the contents of the esophagus, looking for the acidic characteristic of stomach contents being refluxed up the esophagus. The probe may also be used to measure pressures in the esophagus ("manometry") to help determine the usefulness of surgical treatment.
There are other causes of frequent spitting up or vomiting in the infant and child besides GER, such as metabolic or allergic conditions. Should the above tests show that GER is not the cause, then the child's physician may do other tests to isolate the cause.
Treatment of GER
The first line of treatment is usually a combination of positioning and diet changes. In positioning the infant that refluxes, it is best to elevate the head above the level of the stomach. In the 1970s and 1980s, it was common to have the child lie on his stomach (the "prone" position); however, studies in the early 1990s showed that there was an increased risk of Sudden Infant Death Syndrome (SIDS, or "crib death") associated with babies sleeping in the prone position. At the present time, it is considered best to have the refluxing infant lie on his/her side with the head of the bassinet or crib elevated at a 25 to 30 degree angle. For refluxing infants taking formula, the formula can be thickened in order to decrease the total volume that the infant takes at a feeding and to make it harder for the stomach to reflux the thickened liquid. Dry cereal is most often used to thicken the formula, starting at 1 tablespoon for every ounce of formula and going thicker if necessary. Thickening the formula tends to reduce the total volume of contents refluxed as well as increasing calories.
For children or infants that do not respond to these conservative measures, the next step is using medications. This group of drugs are called "prokinetic" drugs. Bethanechol was the first drug used for GER and acted to increase the muscle tone in the esophagus, but was never an approved indication for this drug in the US. It has the significant side effect of increasing bronchospasm in children prone to asthma, and was not that effective in reducing GER symptoms. Metocloperamide (Reglan) is the most common drug used for this condition currently, as it increases the tone of the LES as well as increasing the speed at which the stomach empties into the small intestine. Metocloperamide works better than bethanechol, but still gives mixed results at relieving symptoms. Also, there is a narrow margin between the dose needed for effectiveness and the dose that causes side effects such as sedation and movement disorders. Cisapride (Propulsid) had been a fairly good antireflux medication, but had to be pulled off the market in March 2000 due to side effects involving the heart rhythm. A newer drug called domperidome (Motilin) may be more useful for GER but is not approved for use in the US yet.
For many infants and children with severe GER, acid-reducing products that protect the lining of the esophagus may be useful at decreasing pain. Antacids such as Maalox may be effective, but large and frequent doses are required. More commonly, "anti-secretory" drugs which reduce the amount of acid produced by the stomach are used, such as cimetidine (Tagamet), ranitidine (Zantac), omeprazole (Prilosec) and lansoprazole (Prevacid). These are given together with metocloperamide.
Surgery is used for infants and children with severe GER resistant to medications. These are most often needed in children who reflux so much that they have failed to grow sufficiently or there is chronic respiratory problems such as repeated aspiration pneumonia. Another group of children who often need this surgery are those who have gastrostomy tubes, as the presence of gastrostomy tubes greatly increases the incidence of GER. Fundoplication is the most reliable way to surgically prevent reflux, and is successful more than 90% of the time in published studies. In this procedure, the top of the stomach (the "fundus") is wrapped around the LES; this increases LES pressure and also serves as a valve in preventing GER.
Also see the website:
References:
Buchin PJ, Levy JS, Schullinger JN. Down's syndrome and the gastrointestinal tract. J Clin Gastroenterol 8(2):111-4, 1986.
Hillemeier C, Buchin PJ, Gryboski J. Esophageal dysfunction in Down's syndrome. J Pediatr Gastroenterol Nutr. 1(1):101-4, 1982.
Zarate N, Mearin F, Hidalgo A, Malagelada JR. Prospective evaluation of esophageal motor dysfunction in Down's syndrome. Am J Gastroenterol. 96(6):1718-24, 2001.